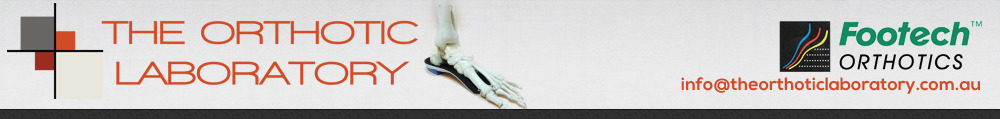
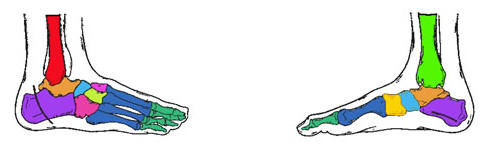
 Your Feet Your Feet
INTRODUCTION TO BIOMECHANICS: Biomechanics is the term used to describe the engineering of human movement. When treating the foot biomechanically we are attempting to improve its function and position with mechanical control. Ideally this is not just support or accommodation but rather the assessment of motions, positions, which are abnormal and result in mechanical symptoms such as corns, calluses, cramps, fatigue, strain etc. and alleviating them by controlling the underlying cause. By directing our management to the cause (aetiology) rather than the effect (pathology) our treatment for these conditions will be much more successful. WHAT IS THE FOOT? The foot is a complex piece of biomechanical engineering comprising 28 bones, over 100 ligaments producing weight bearing, balance and propulsion of the body. It acts not only as the foundation for the body but also its function effects every other motion in the body. Think of the foundations of a house. If two of the main load bearers abnormally shift, the increased load will be placed onto surrounding pillars, and structures above will be placed under tension and strain. Walls may crack and doors may jam along with windows. The house may not fall down but its integrity may be extremely compromised. Similarly shin pain, knee pain, back pain, foot and ankle pain may develop due to a poorly functioning foot and leg alignment. GLOSSARY: Varus
A position of inversion. Valgus
A position of eversion. Pronation
A single motion whose components consist of abduction, eversion and dorsiflexion of one segment or joint in relationship to another Subtalar Varus
An inversion deformity of the posterior of the calcaneus due to its incomplete de-rotation from its infantile position. It is measured with respect to a bisection of the posterior aspect of the calcaneus to the lower one third of the tibia. Rear foot Varus
A combination of subtalar varus and tibial varum resulting in an increased varus attitude of the foot at heel strike. Genu Recurvatum
A posterior hyperextension of the knee, often seen with an equinus deformity. Genu Valgum (Knock Knee)
An attitude of the knee joint in which there is an eversion of the tibia on the femur. This may cause compensation in the subtalar joint, evidenced as supination or increased pronation due to the centre of gravity falling to the medial side of the foot. Genu Varum (Bow Legs)
An attitude of the knee joint in which there is an inversion of the tibia on the femur. This may cause compensation in the subtalar joint evidenced as pronation. Tibial Varum
A deviation of the lower on third of the tibia in the direction of inversion. Torsion
A twist in the long axis of a bone. Malleolar torsion (Tibial torsion)
The angle created by a line extending through the middle of the medial and lateral malleoli in relationship to the frontal plane. If the patient is supine, the angle is created in relationship to the horizontal plane. The normal value would be 13 degrees to 18 degrees. Any amount less than this would represent an internal torsion of the tibia and may result in a toe-in gait. Conversely, any amount greater than this would represent an external torsion of the tibia and may result in a toe-out gait. Femoral Torsion
A twist of the femur between the lower condyles and the neck and head above, which may account for toe-in or toe-out gait. HOW THE FOOT WORKS: During walking the foot has 2 major functions: 1. Mobile Adaptor On initial contact it must be loose and mobile so that it can adapt to different surfaces that it is placed up i.e. flat, angled, smooth, and bumpy but at the same time act as a shock absorber for the leg and body above. 2. Rigid Lever During the middle of foot contact the foot must be transferred into a rigid lever to stabilize and balance the body's weight so as to lift and propel it forward. PHASES OF GAIT There exists 3 basic phases of gait: 1. Contact phase 2. Midstance phase 3. Propulsive phase For the foot to become a mobile adaptor it must "pronate". Pronation is a term used to describe a which, when viewed from behind (posterior) and from the inside (medial), appears to "roll in" (see Glossary of Terms for definition). Timing is of great importance because if the foot is functioning as a mobile adaptor i.e. pronating when it should be a rigid lever (supinating), then it cannot perform its specific function for that phase. In most cases the foot contacts the ground slightly inverted or supinated (rolling out) and then it moves in the direction of eversion or pronation (rolling in). Pronation is a complex motion taking place at the subtalar joint which is between the talus and calcaneous. During the pronation phase the subtalar joint will unlock and so will the midtarsal joint. The midtarsal joint is formed between the talus and calcaneous on onside and the cuboid and medial cuneiform in front. The midtarsal joint visually helps to form the apex of the long arch of the foot. Once these joints are unlocked the entire foot becomes loose and mobile. This continues for the first 25% of the gait cycle and from this time the foot must start to become a rigid lever in prepartion for receiving balancing and propelling the body's weight. To achieve this the foot should start to move out of pronation into the direction of supination i.e. begin to roll out. Pronate and supinate your foot and check these motions. Supination continues for the 2nd 25% of the gait cycle, which brings it to mid stance or 50% of the gait cycle. The foot should now be in its neutral position i.e. neither pronated nor supinated. The subtalar joint will be neutral and the midtarsal joint will be locked and forming a rigid lever in anticipation for balancing, lifting and moving the body's weight. In the normal foot at this point of the gait cycle all the metatarsal heads are firmly planted on the ground and perpendicular to the rear foot. For the remainder of the gait cycle the foot will continue to supinate even as toe-off or the propulsive phase occurs. In the normal foot all bones remain in their proper position and go through a minimal amount of motion. As a consequence symptoms are generally minimised. All movements in the normal foot proceed in sequence, on time and uninterrupted. THE RESULTS OF FAULTY FOOT FUNCTION Now consider the foot which does not pass through the normal sequence of a mobile adaptor to a rigid lever during the gait cycle. Herein lays the basis for over 90% of the mechanical symptoms evidenced in the foot and which contribute to a large percentage of leg related mechanical symptoms. Examples of such symptoms with faulty feet are: Retracted toes (hammer toes, claw toes) Heloma durum (hard corns) Callouses Metatarsalagia (forefoot pain) Morton's neuroma (pinching of a nerve, typically between 3rd and 4th metatarsal heads) Heel spurs (plantar fascitis, general heel pain) Foot strain and general foot tiredness Metatarsal bursitis Bunions (hallux Abducto Valgus) Sever's condition (heel pain in children) Stress fractures Arthritis ie Hallux Limitus etc Examples of such symptoms in the legs are: Achilles tendonitis Tibialis Posterior tendonitis Sinus Tarsi Syndrome (lateral subtalar joint compression) Shin splints Tibia and Fibular stress fractures Patello femoral pain (knee cap related pain) Lower leg fatigue Growing pain in children This list is by no means complete but does highlight common mechanical symptoms of faulty feet or legs. What generally happens with these symptoms is that the foot is loaded with the body's weight and stress (i.e. compression, shearing and tensile forces) at the time when the foot is not in a position to receive it. The foot is not stable and the bones and joints which are being subject to load are free to move in abnormal directions through abnormal range of motion. The foot cannot become fixed with stability against the ground or efficiently propel the body's weight. With this in mind, stabilizing leg and foot muscles are now forced to work harder and longer, with the result being muscle fatigue and tiredness. Twisting and shearing of bones and joints may result in internal inflammation of soft tissue, joints and the skin, the latter which we see as lesions in the skin; i.e., corns and callous. Torsional or rotary stresses transmitted through the legs to the pelvis and spine may produce back, pelvis and leg postural complaints. Bones which are subjected to more stress and load that they can physiologically tolerate may actually change their shape in an attempt to better tolerate and cope with these pathological stresses; i.e. heel spur formation. This phenomenon is known as Functional Adaptation of Bone and occurs normally or abnormally throughout the body. A good analogy is the tyres of your car if they are out of alignment there will be a rapid and uneven wear pattern of them. However if we re-establish correct alignment the forces causing the abnormal wear and tear will be normalised and damage will cease. To a large degree the same principal can be applied to the foot and leg alignment. Whilst we cannot replace our feet as we can replace our car tyres, by normalising our foot mechanics the body is able to repair inflamed tissue; providing the damage is not excessive. In order to halt the progress of damage caused by faulty function of the foot and leg and obtain repair when possible we must enable the foot to function as close as possible to a neutral position. This will enable optimal efficient function. |